- Denis, Daniel; Shedid, Daniel (2014). "Cervical spondylosis: a rare and curable cause of vertebrobasilar insufficiency". Eur Spine J. 23: 206–13.
- Newman & Santiago, 2013
- Caridi, John M; Pumberger, Matthias; Hughes, Alexander P (2011). "Cervical Radiculopathy: A review". HSS J. 7 (3): 265–272.
- Lhermittev, JJ (1920). "Les Formes Douloureuses de la commotion de la moelle épiniére". Rev Neurol. 36: 257–262.
- McCormack, Bruce M (1996). "Cervical Spondylosis an update". Western Journal of Medicine. 165 (1/2): 43–44. PMC 1307540.
- Binder, Allan (2007). "Cervical Spondylosis and Neck Pain". British Medical Journal. 334 (7592): 527–31.
- Gibson, JNA; Waddell, G (2005). "Surgery for degenerative lumbar spondylosis". Cochrane Database of Systematic Reviews (4): CD001352.
- Malcolm, George (2002). "Surgical disorders of the cervical spine: presentation and management of common disorders". J Neurol Neurosurg Psychiatry. 73 (Suppl 1): i34–i41.
Spondylosis: What Are Those Spinal Bony Projections, Their Causes and Symptoms
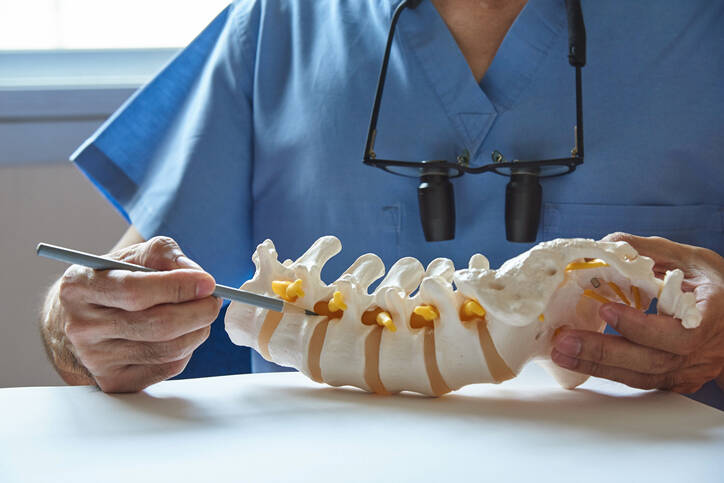
Spondylosis is classified as a degenerative disease of the spine. It affects any part of the spine and is a source of other symptoms besides back pain. It is a common problem, especially in middle and older age.
Most common symptoms
- Shoulder Blade Pain
- Feeling of heavy legs
- Chest pain
- Flank Pain
- Headache
- Limb pain
- Nerve pain
- Leg Pain
- Painful Breathing
- Shooting pain in fingers and toes
- Pain that Radiates into the Shoulder
- Groin Pain
- Back Pain
- Spirituality
- The Hump
- Tinnitus
- Muscle stiffness
- Defence
- Tingling
- Muscle weakness
- Head spinning
Characteristics
This degenerative process affects any part of the spine, from the neck through the thoracic or cervical spine. However, it can affect the entire spine at once.
It is one of the common ailments that are the source of back pain, but also of other discomforts. These are neurological in nature.
Spondylosis occurs mainly in middle-aged and elderly people. Since it is a degenerative change, which is also conditioned by advancing age.
The extent of the damage extends to the entire spinal segment. From the vertebrae, to the intervertebral disc, to the articular surfaces and other structures such as ligaments.
To better cover or illustrate the issue, we also provide brief information about the spine.
Spine, vertebrae, discs, joints and ligaments
The spine serves as the support of the human body. In addition to bearing weight, it also serves in movement, which it provides in a wide range. The spinal cord runs across the spine and protects it from damage.
The spine consists of 33 to 34 vertebrae.
The vertebrae are connected to each other. This connection is fixed but movable. It is made up of a number of structures and mechanisms.
The connection of the vertebrae is ensured by several mechanisms:
- ligaments - the ligamentous apparatus that connects the individual vertebrae, but also the entire spine
- short ligaments of the spine - between the vertebrae
- long ligaments of the spine - along the spine
- intervertebral joints - articular surfaces of vertebrae
- intervertebral discs - used for movement and shock absorption of the vertebrae during movement
- special connection - examples are cartilage or other non-movable connections, such as the sacrum
- back muscles - they are used for fixation, but also for movement, and in addition to the muscles of the spine, the muscles of the abdomen or pelvis are also important
The vertebrae are...
Vertebrae are bones. They carry the weight of the body, they are also important in movement.
There are 33 or 34 of them, and their interconnection allows mobility of the spine. The individual vertebrae are designated according to their location, from the neck to the coccyx.
Table: individual sections of the spine and vertebrae designation
| Segment | Latin name | Description |
| Cervical spine | vertebrae cervicales |
|
| Thoracic spine | vertebrae thoracicae |
|
| Lumbar spine | vertebrae lumbales |
|
| Sacral spine | vertebrae sacrales |
|
| Coccyx | vertebrae coccygeae |
|
The specific shape of the vertebrae allows mobility of the spine and also forms a supporting skeleton for the body.
An example is the spinal canal (canalis vertebralis), through which the spinal cord passes. This is formed by the vertebral foramina of the cervical, thoracic and lumbar vertebrae.
The vertebra is made up of several anatomical structures such as the body, the arch or the process.
Vertebral body
The Latin name us corpus vertebrae - it forms the front part of the vertebra. It has mainly a weight-bearing function.
The vertebral bodies have different heights. Among the largest vertebrae are the cervical vertebrae, on the contrary, the thinnest ones are located in the cervical spine section.
The top and bottom surfaces of the vertebral body are flat and the intervertebral disc adapts to its shape.
Vertebral arch
In one part it connects to the body of the vertebra with small connections referred to as pedicles.
The second part of the arch is the plate. On both sides it forms the vertebral aperture through which the spinal cord passes.
Pedicles are also important from an anatomical point of view because of their small notches. These form the intervertebral openings through which the spinal nerves pass.
Vertebral processes
The processes are another important part of the vertebra. They protrude from the arch. They are important in the joining of the vertebrae, but also in the movement of the spine.
The vertebrae have three types of processes, namely:
- spinous process, processus spinosus, runs directly to the rear
- there is only one such process and it can be felt on the back under the skin
- these processes are also connected to the tendons of the muscles
- transverse process, processus transversi - it is paired
- muscle strengthening
- in the thoracic part of the ribs
- articular process, processus articulares, it is paired
- at the point behind the foot of the arch of the vertebra
- the articulation of the vertebrae is located here
- consists cartilage
Intervertebral disc
It gets its name disc from the Latin name disci intervertebrales.
They are located between the vertebrae. They attach to the bodies of the vertebrae and follow their shape.
They are flexible but also rigid, which ensures their shock-absorbing function as well as the movement itself.
The main functions of the intervertebral discs are:
- shock absorption - walking, running, jumping and movement in general
- stabilisation of the spine
- maintaining balance
- equalize compressive and tensile forces
- they spread them over the entire surface of the disc and vertebrae
- they are involved in every movement of the spine, bending and rotation of the body
Like the vertebrae, the discs vary in size. They are lower in the cervical region, but higher in the cervical region.
Number of intervertebral discs = 23.
The discs fill the intervertebral spaces from vertebrae C2 - C3 to L5 and S1.
Table: composition of the intervertebral disc
| Segment | Latin name | Description |
| Ring | Anulus fibrosus |
|
| Nucleus | Nucleus pulposus |
|
| Endplate | Vertebral endplate |
|
Intervertebral discs are under load throughout life. Static, but also dynamic forces act here.
Uneven overload of the spine leads to changes over time that are the cause of back pain and other neurological problems.
As can be seen from the table, the disc, more precisely its nucleus, is not supplied with blood - nutrients.
Nutrition occurs during movement.
The alternation of tension and relaxation of the disc creates a flow and expulsion of fluid with nutrients and waste substances. This phenomenon is especially beneficial when walking.
Conversely, inactivity and a sedentary lifestyle affect negatively, due to a reduced rate of fluid flow. Which has an impact on the nourishment of the discs and, ultimately, on their functionality.
Intervertebral joints
The Latin name is articulationes intervertebrales. Their main task is to provide movement between the vertebrae.
They are located between the processes of the cervical, thoracic and lumbar vertebrae. They vary in shape and size according to the section of the spine in which they are located.
They are shorter in the thoracic section of the spine - here the range of motion is also lower.
Intervertebral joints + intervertebral disc compression capability = functional unit.
Movement into forward bending, backward bending, sideways bending as well as rotation, i.e. rotation and, to a certain extent, springing movement are provided.
Why are we presenting all this information, you ask?
Spondylosis affects the area of the vertebra and its segment or several parts of the spine.
So what is spondylosis?
Spondylosis = degenerative process.
It affects the vertebral body, discs, joints, but also the ligaments and affects the microcirculation, i.e. the blood supply.
Degenerative changes mostly begin to manifest in middle age and old age. Until this time, they may proceed asymptomatically.
With age, the ratio of water in the disc changes.
This will cause the height of the disc to decrease. This change in the overall length of the segment causes a length disparity with respect to the ligamentous fibres.
The result is instability of the vertebral segment. This is compounded by improper load distribution on the disc and vertebral body.
Pathological process affecting the intervertebral disc = osteochondrosis.
Disability of the small intervertebral joints = spondyloarthrosis.
This pathologically altered process causes minor injuries (microtraumas, microtraumas) at the level of the vertebral body and the disc. The destroyed structures are not healed by the original tissue.
Poškodené tkanivo nahrádza kostná hmota - osteophyte = bony projection.
Osteophytes can take different shapes. They are asymmetrical, thinner or thicker, shaped for example into spines, beaks, even, they can form a bridge of the disc. This bridging is actually the fusion of two vertebrae, which results in the immobilisation of the part in question.
Sclerotization of the vertebral body - changes in the structure of the vertebra may be associated.
It is also reported that through this process the body tries to compensate for instability in the vertebral segment, which is caused by hypermobility of the intervertebral joints and narrowing of the width of the disc.
Osteophytes can cause irritation of surrounding structures, as well as nerve tissue and spinal nerves (less commonly). Hence the association with pain and other neurological complaints.
They are most often formed in places with a higher range of motion of the spine.
In the lower cervical, thoracic and cervical spine.
Causes
However, certain factors also contribute to the progression (advancement) of the condition. These can be genetic predisposition and family history.
Nowadays, improper lifestyle is increasingly cited as the main source of spinal problems.
Of course, since a sedentary lifestyle reduces the rate of nutrient transfer to the intervertebral disc. This in the long term has a negative impact on proper function.
Risk factors involved in spondylosis:
- age
- onset when middle-aged
- culminating in old age
- genetic predisposition and family history
- sedentary lifestyle
- metabolic diseases
- injury
- diseases of the cardiovascular system
- disorders of blood circulation and vascular permeability
- overloading of the muscles and ligaments of the spine
- long-term unilateral load
- workload and hard work
- lifting loads
- incorrect lifting technique
- sedentary work
- long-term driving
- poor posture and inappropriate movement habits
Symptoms
X-ray finding:
in 45-year-olds approximately 50%
in 60-year-olds in more than 90%.
Growths can be the cause of irritation of surrounding structures. Less often, posterior processes are involved in nerve root irritation, especially in the case of cervical spondylosis.
In the case of spondylosis, pain occurs. The pain is mostly mild and has a fluctuating character.
Pain is aggravated by prolonged standing, sitting, persistence in one position (at work), but also by physical exertion.
The presence of symptoms affects the location of spondylosis and its extent.
Example: cervical spondylosis
The name already implies that it is a degenerative process that affects the cervical part of the spine.
With significant narrowing of the intervertebral space, nerve oppression may occur due to certain movements.
In the most serious conditions, the space through which blood vessels carry blood to the spinal cord or brain may be restricted.
Consequently, there is a problem with sufficient blood supply to the affected area.
The pain is mostly mild, it can be long-lasting or recurrent. Neck stiffness is associated.
Difficulties may radiate to the back of the head, shoulders and upper limbs. Radiation of pain may be to one or both upper limbs into the shoulder, up through the forearm into the hand.
Thus, in spondylosis, radiculopathy can also arise, which is an irritation of the nerve root. It is reported to most commonly affect the C6 and C7 cervical segment area.
In this case, the pain occurs in the neck, radiates to the upper limbs, between the shoulder blades or even to the chest. It is accompanied by trembling or tingling - paresthesias, weakening or impaired sensitivity. Plus, associated muscle weakness in the neck and adjacent limb.
More details in the article: Radiculopathy
Spondylosis affecting the lumbar spine is referred to as lumbar spondylosis. It accounts for approximately 10-12% of all spondylosis cases.
Diagnostics
A physical examination is important. The neurological examination, as with all spinal problems, looks at posture, gait, range of motion, or overall posture and movement. The specialist examines reflexes and manoeuvres.
Imaging methods such as X-ray, CT + myelography or magnetic resonance imaging are important. EMG - electromyography, i.e. the measurement of electrical potentials and muscle activity, is added.
It is important to distinguish spondylosis from another disease - differential diagnosis. Therefore, laboratory examination of the blood is also advisable. Examination of bone tissue - densitometry.
In differential differentiation, it is necessary to think about other diseases, such as:
- ankylosing spondylitis - Bechterev's disease
- inflammation of the spine
- spondylopathy
- spondylolisthesis
- osteoporosis
- injury
- migraine or tension headache
- amyotrophic lateral sclerosis or multiple sclerosis
- and others
Course
The mild degree of spondylosis is mostly asymptomatic.
Depending on the extent of damage to the vertebral segment, difficulties may be added. An example is pain, which can also be long-lasting or recur in periods of time.
Pain can be aggravated by prolonged sitting, standing, staying in one position or physical exertion. Therefore, it intensifies during the day, to the detriment of all-day exertion.
To the pain is added restriction of mobility of the part in question. Alternatively, the pain may radiate to other areas, such as to the limbs.
When the cervical vertebrae are affected, it will be to the upper limb. In the case of involvement of the cervical region, it will be to the lower limb.
The course is directly dependent on the extent of disability.
If the bone growths significantly restrict the space, more serious neurological problems may arise. These subsequently manifest as radicular syndrome.
Pain is accompanied by paresthesias, i.e. tingling, and muscle weakness.
The cervical spine is the most flexible section of the spine. Pain from this area can propagate - spread to the upper limb. But also to the head, to the chest or between the shoulder blades.
The thoracic spine is relatively rigid, thanks to the ribs and rib cage. In this area, pain due to spondylosis is less common. If, so pain occurs, for example, with radiation to the chest and over the ribs.
Spondylosis in the lumbar region can spell trouble for possible oppression of the plexus of nerves.
Then the pain occurs in the groin and sacrum or in the buttock area. It moves to the lower limbs. In radiculopathy, there is also a sensory impairment and muscle weakness in the leg.
Pain in the sacrum with transfer through the buttocks can also indicate sciatica - inflammation of the sciatic nerve.
Table: possible difficulties in damaging individual sections
| Spinal segment | Description of signs and symptoms |
| Cervical (neck) |
|
| Thoracal (chest) |
|
| Lumbar (lower back) |
|
|
Remember that mild forms may be asymptomatic or mild.
Or...
Severe degenerative disability. This can lead to spondylogenic myelopathy, an impairment of sensation, mobility and reflexes. | |
Although the milder form does not cause significant difficulties, appropriate and early treatment is important. Of course, rehabilitation and sufficient physical activity are necessary. The aim is to prevent progression of the disease, which can lead to disability at a later stage.
How spondylosis is treated is described in the section on treatment.
How it is treated: Spondylosis
Treatment of spondylosis: Medication, exercise, rehabilitation to surgery
Show moreSpondylosis is treated by
Other names
Interesting resources










