- International Trauma Life Support for Emergency Care Providers (8 ed.). Pearson Education Limited. 2018. pp. 172–73. ISBN 978-1292-17084-8.
- ATLS – Advanced Trauma Life Support – Student Course Manual (10 ed.). American College of Surgeons. 2018. pp. 43–52, 135. ISBN 978-78-0-9968267.
- Tabas, Jeffrey; Reynolds, Teri (2010). High Risk Emergencies, An Issue of Emergency Medicine Clinics (E-book). Elsevier Health Sciences. p. 58. ISBN 978-1455700257.
- Smith, N; Lopez, RA; Silberman, M (January 2019). "Distributive Shock". PMID 29261964.
- Olaussen A, Blackburn T, Mitra B, Fitzgerald M (June 2014). "Review article: shock index for prediction of critical bleeding post-trauma: a systematic review". Emergency Medicine Australasia. 26 (3): 223–28. doi:10.1111/1742-6723.12232. PMID 24712642. S2CID 19881753.
- Guyton, Arthur; Hall, John (2006). "Chapter 24: Circulatory Shock and Physiology of Its Treatment". In Gruliow, Rebecca (ed.). Textbook of Medical Physiology (11th ed.). Philadelphia, Pennsylvania: Elsevier Inc. pp. 278–88. ISBN 978-0-7216-0240-0.
- Tintinalli, Judith E. (2010). Emergency Medicine: A Comprehensive Study Guide. New York: McGraw-Hill Companies. pp. 165–72. ISBN 978-0-07-148480-0.
- Tintinalli, Judith E. (2010). Emergency Medicine: A Comprehensive Study Guide. New York: McGraw-Hill Companies. pp. 174–75. ISBN 978-0-07-148480-0.
- Assessing dehydration and shock. NCBI Bookshelf. National Collaborating Centre for Women's and Children's Health (UK). April 2009. Retrieved 2019-05-09.
- Silverman, Adam (Oct 2005). "Shock: A Common Pathway For Life-Threatening Pediatric Illnesses And Injuries". Pediatric Emergency Medicine Practice. 2 (10).
Shock: Medical Definition, Causes, Types and Stages

Shock - informally, this term is mostly used to indicate a stress response. However, in medicine, it has a completely different meaning. It indicates a condition where a person is acutely at risk to health and life.
Most common symptoms
- Malaise
- Sweating
- Chest pain
- Apathy
- Abdominal Pain
- Headache
- Spirituality
- Fever
- Increased body temperature
- Nausea
- Head spinning
- Tinnitus
- Black stool
- Bleeding
- Blue leather
- Indigestion
- Low blood pressure
- Lung Island
- Swelling of the limbs
- The Island
- Disorders of consciousness
- Slowed heartbeat
- Cold extremities
- Muscle weakness
- Pressure on the chest
- Anxiety
- Vomiting
- Vomiting blood
- Urinary retention - anuria/retentiveness
- Blurred vision
- Deterioration of vision
- Yellowish skin
- Confusion
- Accelerated heart rate
Characteristics
FAQ:
What does shock mean in medicine?
What could be the cause?
What types and stages of shock do we know?
How does it manifest itself?
Shock refers to the body's overall response, which occurs for several reasons. The shock condition affects various body systems and manifests itself in a variety of symptoms. It endangers a person's health and life.
What is a Shock? How is it Defined?
When looking for a definition of shock, we can come across several forms. Their essence is the same, only the way of expression changes.
Shock is...
1.
... a disproportion between the need and supply of oxygen and nutrients for the body.
2.
... a life-threatening condition based on a disorder of the blood supply to cells, tissues and organs. If left untreated, organs and organ systems gradually fail. It affects vital organs, such as the brain, heart or kidneys and lungs.
3.
... is an acute, i.e. sudden, or even subacute change in macrocirculation and microcirculation, which is manifested by reduced blood flow to tissues and organs. There is insufficient oxygen and nutrients in the cells. Toxic metabolic or metabolite products accumulate in them.
Hypoxia - the body or a region of the body is deprived of adequate oxygen supply at the tissue level.
Subsequently, it progresses to a malfunction of the cells, organs and finally the entire organ systems. In case of treatment delay, it goes into an irreversible, ie irreversible phase. Damage to the brain, heart, kidneys and other organs occurs.
The fcondition ends in the death of the victim.
4.
... is a severe dynamic condition in which the supply of oxygen to the tissues of vital organs is insufficient for their current energy requirements.
Excess post-exercise oxygen consumption, informally called afterburn or "oxygen debt", occurs and metabolic acidosis develops.
Learn more on acidosis and alkalosis in the article Acidification is nonsense.
The cause is a disparity between the size of the vascular circulatory system and the amount of blood, i.e. fluids in the bloodstream.

The 3 Phases of Shock
The shock is said to be a dynamic state because it goes through several stages. This division is especially important from the point of view of treatment.
The shock has three phases, which are also referred to as compensatory shock, decompensated shock, and refractory shock. The transition from one phase to another is dynamic and the speed depends on several factors.
The rate of shock development depends on:
- the state of the organism at the time of the acute change
- age
- comorbidities
- immunity
- coagulation
- CNS - central nervous system
- mental state
- the extent of the cause
- the time of the event
- the presence of negative factors, such as fatigue or hypothermia
Table: Individual phases of shock
| Shock phase | Technical description |
| Compensatory | Compensatory shock
|
| Decompensated | Decompensated shock
|
| Refractory |
Terminal phase, i.e. final, irreversible
|
Necrosis, i.e. cell decay = cell death.
If cell death affects a certain number of cells of vital organs...
...eliminating the root cause of the shock will not help either.
The essence of the irreversible phase of shock.
Causes
And plus, for impaired drainage of toxic substances that arise during metabolism and impaired function from cells.

There may be various causes of shock.
1. The reason may be the loss of fluids from the bloodstream.
It occurs due to bleeding, significant burns or severe dehydration. It is generally referred to as hypovolemic shock.
2. The second cause may be reduced performance and heart failure.
Which is also a cardiogenic shock. Which can occur with a heart rhythm disorder or a heart muscle infarction. Another subtype is obstructive shock, which arises on the basis of pericardial tamponade.
3. The third major category is vascular bed enlargement.
Simply put, when the blood vessels are excessively dilated. It's called a distribution shock. It occurs, for example, in anaphylaxis, such as anaphylactic shock, or severe sepsis.
Sepsis, septic condition, septicemia - informally called blood poisoning - which is a severe infection in which pathogens spread blood throughout the body.
The risk of shock also occurs in conditions such as:
- diabetic coma - hyperglycemic coma, but also hypoglycemic coma
- thyroid dysfunction
- renal failure
- acute liver failure
- liver cirrhosis decompensation
- intoxication
- extensive injuries
- long surgery
Classification of Shock by Cause
The shock is divided according to the cause.
Table: types of shock
| Main category | Shock name | Cause |
| Insufficient fluid in the vascular bed - lack of blood | Hemorrhagic |
due to bleeding that may occur, for example, when:
|
| Traumatic | due to injuries:
| |
| Burn |
occurs in all severe burns
| |
| Hypovolemic |
with a reduced volume of fluid in the body, if sufficient replacement of lost fluids is not ensured
| |
| Generally, but inaccurately, this category is referred to as hypovolemic shock. It occurs when the volume of circulating blood is reduced by more than 25-30% in 30 minutes - or with a small but long-term blood loss. When the femur is broken, the femur can receive up to 1 liter of blood - there is an enlargement of about 1 cm in circumference. | ||
| Low cardiac output per minute Decreased heart function as a pump. The amount of blood expelled from the heart decreases. There is enough blood in the blood vessels. | Cardiogenic |
|
| Obstructive |
| |
| Peripheral disorder It is also referred to as a distributive shock. There is enough blood in the blood vessels, the cause is not bleeding or heart's pumping dysfunction. | Anaphylactic | in case of a severe allergic reaction, i.e. anaphylaxis, for example after allergy to:
|
| Toxic | in chemical intoxication, but also in pancreatitis | |
| Septic | Sepsis, blood poisoning, as a complication of some infections, even with burns | |
| Neurogenic | For brain and spinal cord injuries - especially in the neck and chest areas | |
| Endocrine | in case of impaired endocrine glands | |
Symptoms
In case of treatment delay or failure up to the refraction phase. At this point, there will be a failure of the organs and entire systems and their damage. It ends in death.
Shock has general manifestations:
- restlessness, anxiety
- weakness, fatigue and drowsiness
- dizziness
- visual impairment
- nausea, feeling sick - nausea to vomiting
- pale skin
- cold skin
- excessive sweating - sticky and cold sweat
- acceleration of heart rate, heart rate
- the pulse is fast and difficult to feel - weak, barely palpable pulse
- rapid breathing
- feeling short of breath
- disorder of consciousness at a later stage - unconsciousness

Table: Distribution of shock symptoms according to the organ system
| Systemic organ | Symptoms |
| Respiratory |
|
| Cardiovascular |
|
| Skin |
|
| Nervous - brain - mental state |
|
| Excretory |
|
| Digestive |
|
Classification of Shock According to Clinical Severity
From this point of view, the shock is divided into mild, moderate, severe and terminal shock.
1. Mild shock
The person is weak, tired, generally depressed. The person is still conscious and has a pale, cold skin, dry mouth and is thirsty.
The skin is cold to the touch, moist and sweaty.
The activity of the heart accelerates, which we can observe as an accelerated pulse - approximately 90-100 pulses per minute. So far, the blood pressure is above 100 mmHg.
Learn more on blood pressure values in a clear table.
Bleeding may involve blood loss in the range of 1000 - 1200 ml = 20 - 25% of the volume of circulating blood.
2. Moderate shock
The mental state is deteriorating, the person is apathetic, he is not interested in the environment.
The skin is very pale - "as white as a sheet". Typically, it is cold, sticky and sweaty.
The heart rate increases to 110-120 pulses per minute - tachycardia. And at this stage, the blood pressure is also falling, with a value of less than 100 mmHg - which is called hypotension.
Learn more: Low blood pressure - hypotension.
Approximate blood loss can be estimated at 1500 - 1700 ml of blood = 30 - 35% of the circulating blood volume.
3. Severe shock
The person's mental state deteriorates and he/she is significantly weak and apathetic, moight be nauseous (feeling sick) or vomit.
The skin has a grayish tinge, associated with cyanosis - bluish-purple skin hue. We can observe it on the fingers, lips but also on the ears and the tip of the nose.
The pulse rises above 120 - 160 per minute. Blood pressure, on the other hand, drops below 80 mmHg.
In this case, blood losses can be estimated at 2,000 milliliters.
4. Terminal shock
It is the last stage of shock. The person is in immediate danger of life.
There is a disorder of consciousness - loss of consciousness, coma.
The skin is mottled. The pulse impalpable and the blood pressure at this point cannot be measured.
Irregular breathing to shallow breathing are a sign of the approaching end.
Blood loss at this stage is estimated at over 2,500 millilitres - which is 50% of the volume of circulating blood.
Diagnostics
With delayed treatment, there is a risk of the shock deepening into its irreversible form and into the terminal stage, ie the death of a person.
Diagnosis includes:
- medical history, i.e. ask the patient whether there is pain (for example on the chest, abdomen), subjective perception of the quality of respiration, the onset of difficulties
- clinical picture, that is, how the difficulties manifest themselves
- physical examination - blood pressure, pulse, respiratory rate, blood oxygen saturation and others
- blood and urine collection for laboratory examination
- blood count, hemocoagulation, mineralogram, inflammatory markers, acid-base balance, biochemistry
- imaging methods
- ECG, ultrasound, X-ray, CT, MRI, sonography
- coronary angiography in case of cardiac problems
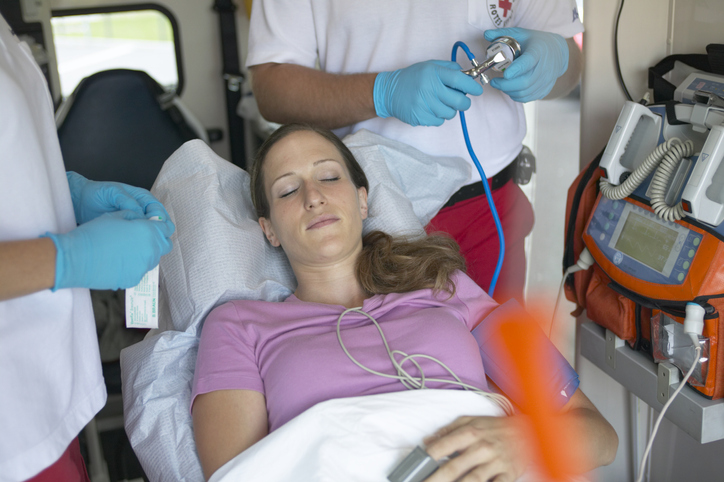
Shock index
The Shock Index is used to indicate the level of occult shock.
The ratio between systolic pressure (sTK) and pulse frequency (P):
- Normal condition = 1,5
- which is the result of the ratio
- 60 P per minute : 120 sTK
- 60 : 120 = 1,5
- Advanced shock = 1,0
- 100 P per minute : 100 sTK
- 100 : 100 = 1
- Severe shock = 2,0
- 120 P per minute : 60 sTK
- 120 : 60 = 2,0
Course
Hypovolemic Shock...
It is characterized by a reduction in venous return.
It is also referred to as cold shock.
This means that the amount of blood flowing from the body back to the heart is reduced. As a result, the heart rate increases.
There is an increase on two levels, and thus an acceleration of the frequency - tachycardia, as well as an increase in the strength of contraction - inotropic state. Vascular resistance increases as well - due to vasoconstriction.
The role of this mechanism is to maintain blood flow to vital organs such as the brain and heart.
To centralise the circulation, the vessels narrow - vasoconstriction, the frequency accelerates. Significant hypotension occurs when approximately 20% of the circulating fluid volume is lost. Deceleration of the heart (bradycardia) is a sign of a late stage.
Cardiogenic Shock...
It is caused by reduced blood flow to tissues and organs. The reason is a reduction in the heart's ability to pump blood.
The minute volume of the heart decreases.
There is enough blood in the bloodstream.
Low blood pressure, decreased cardiac output, and tachycardia are also associated. Due peripheral vasoconstriction, i.e. narrowing of blood vessels in peripheral organs and tissues, the production of urine is reduced, the skin is pale, cold, sweaty, there is also muscle weakness and a change in the psyche.
Up to 75% are due to acute myocardial infarction.
On the basis of decompensated ischemic heart disease.
Another example is heart failure.
Distributive Shock...
In this form of shock, there is no vasoconstriction - narrowing of the blood vessels, but, conversely, vasodilation - which is a widening of blood vessels.
Even in this case, the amount of circulating blood is preserved.
The skin remains warm.
Warm skin, and thus increased body temperature, is caused by infection - pathogenic organisms in septic shock.
Sepsis is also associated with symptoms such as:
- fever
- skin feels hot
- pinkish skin
- chills
- nausea
- vomiting
- increased leukocyte count
- restlessness to disorientation
- hyperglycaemia (high blood sugar) or hypoglycaemia (low blood sugar)
Sepsis is a Systemic Inflammatory Response Syndrome - SIRS to various stimuli. An example is bacterial infection, but also pancreatitis. It usually develops in the elderly and in people with comorbidities.
This type of shock is also referred to as warm shock.
Heart function is preserved throughout.
Later on, due to leaching of toxic substances, heart function deteriorates. Acidosis (shift of the pH of the internal environment towards acidic), hypoxemia (reduction of blood oxygenation), hypoxia (low tissue oxygenation) occur.
Toxic Shock Syndrome (TSS)
TSS from Staphylococcus infections was identified in the late 1970s and early 1980s when highly absorbent tampons were widely used by menstruating women.
Other causes include infection of surgical wounds, various abscesses, infection of burns, conjunctivitis.
It occurs in the presence of symptoms such as:
- fever
- low blood pressure
- vomiting
- diarrhea
- muscle pain
- decreased kidney function
- changes in the psyche, apathy, confusion
- widespread rash - exanthem
- redness of the conjunctiva
- coated tongue
Anaphylactic Shock
Of all the distributive forms, anaphylactic shock develops fastest, meaning within about 30 minutes of contact with the allergen.
It is the most severe form of allergy. For example, it occurs after applying medication, digesting food or an insect bite.
Signs and symptoms arise very quickly.
Anaphylactic shock occurs with:
- severe widening of blood vessels - vasodilation
- swelling due to increased vascular permeability
- skin manifestations such as hives - urticaria, redness
- pallor and cyanosis
- low blood pressure due to reduced cardiac output
- common cold
- nausea or vomiting
- abdominal pain - cramps
- constriction of the muscles in the walls of the bronchiole - bronchospasms
- eventually circulatory failure, pulmonary edema
Neurogenic Shock
Neurogenic shock occurs through the presence of the triad of symptoms, namely hypotension (low blood pressure), bradycardia (decrease in heart rate) and hypothermia (decrease in body temperature). Vasodilation, i.e. the widening of blood vessels, is also present.
The cause may be vagotonia, ie irritation of the vagus nerve - a wandering nerve, deep general anesthesia, exaggerated emotions - fear, brain damage or bloodless spinal cord.
A spinal shock is different in that it occurs when the spinal cord is injured.
In spinal shock, sympathetic stimulation is increased, which is manifested by a sudden high blood pressure, with a high or low heart rate. High blood pressure is replaced by a drop in blood pressure, even in the long term.
How it is treated: Shock - State of shock
Shock treatment: By type + shock first aid
Show moreShock, Pathology of Different Types, Animation
Shock - State of shock is treated by
Shock - State of shock is examined by
Other names
Interesting resources










