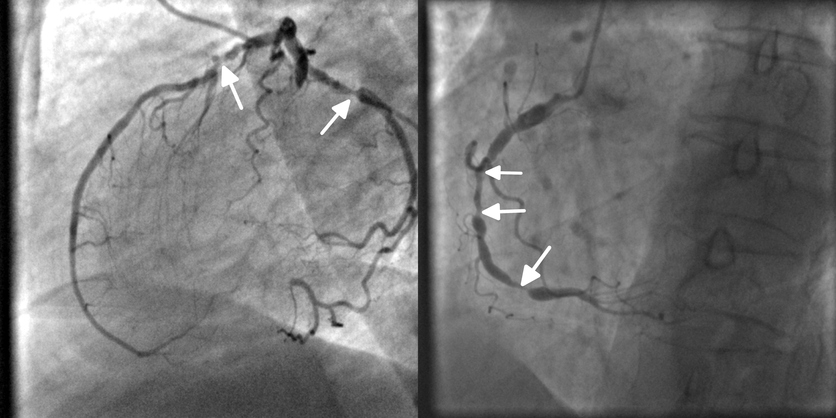
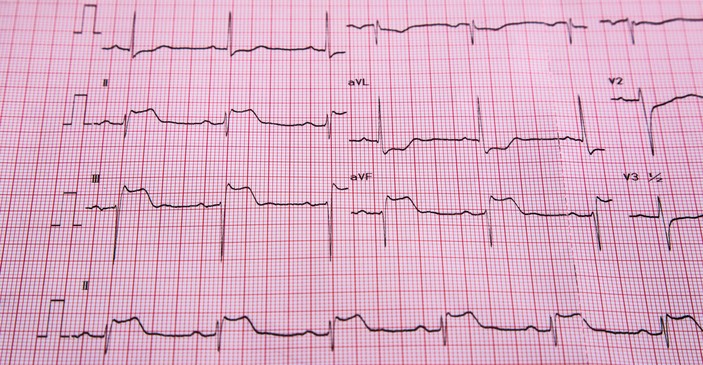
- "Coronary heart disease – causes, symptoms, prevention". Southern Cross Healthcare Group.
- Faxon DP, Creager MA, Smith SC, Pasternak RC, Olin JW, Bettmann MA, et al. (June 2004). "Atherosclerotic Vascular Disease Conference: Executive summary: Atherosclerotic Vascular Disease Conference proceeding for healthcare professionals from a special writing group of the American Heart Association". Circulation. 109 (21): 2595–604.
- MedlinePlus Encyclopedia: Coronary heart disease
- "What Are the Signs and Symptoms of Coronary Heart Disease?".
- "Coronary Artery Disease (CAD)".
- Mendis S, Puska P, Norrving B, eds. (2011). Global atlas on cardiovascular disease prevention and control. World Health Organization. pp. 3–18.
- Mehta PK, Wei J, Wenger NK (February 2015). "Ischemic heart disease in women: a focus on risk factors". Trends in Cardiovascular Medicine. 25 (2): 140–51.
- "How Is Coronary Heart Disease Diagnosed?".
- "How Can Coronary Heart Disease Be Prevented or Delayed?".
- "How Is Coronary Heart Disease Treated?".
- Vos T, Allen C, Arora M, Barber RM, Bhutta ZA, Brown A, et al. (GBD 2015 Disease and Injury Incidence and Prevalence Collaborators) (October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602.
- Wang H, Naghavi M, Allen C, Barber RM, Bhutta ZA, Carter A, et al. (GBD 2015 Mortality and Causes of Death Collaborators) (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544.
- Bhatia SK (2010). Biomaterials for clinical applications (Online-Ausg. ed.). New York: Springer. p. 23. ISBN 9781441969200.
- "Myocardial ischemia - Symptoms and causes". Mayo Clinic.
- "Ischemic Heart Disease". National Heart, Lung, and Blood Institute (NHLBI).
Ischemic heart disease: Causes and symptoms of coronary heart disease?
Photo source: Getty images
Most common symptoms
- Shoulder Blade Pain
- Malaise
- Chest pain
- Abdominal Pain
- Shooting pain in fingers and toes
- Pain that Radiates into the Shoulder
- Spirituality
- Blue leather
- Sweating
- Nausea
- Low blood pressure
- Lung Island
- Swelling of the limbs
- Disorders of consciousness
- Anxiety
- Slowed heartbeat
- Muscle weakness
- Pressure on the chest
- Head spinning
- Fatigue
- Vomiting
- High blood pressure
- Confusion
- Accelerated heart rate
Show more symptoms ᐯ
How is ischemic heart disease treated: medications, angioplasty, BY-PASS?
Show moreIschemic heart disease is treated by
Ischemic heart disease is examined by
Other names
Coronary artery disease (CAD), coronary heart disease (CHD), ischemic heart disease (IHD), myocardial ischemia, heart disease, atherosclerotic heart disease, natherosclerotic vascular disease, coronary heart disease