- Freedberg, Irwin M.; Fitzpatrick, Thomas B. (2003). Fitzpatrick's dermatology in general medicine (6th ed.). New York: McGraw-Hill. pp. 427–436. ISBN 978-0-07-138076-8.
- James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Saunders. p. 194. ISBN 978-0-7216-2921-6.
- Ritchlin, CT; Colbert, RA; Gladman, DD (March 2017). "Psoriatic Arthritis". New England Journal of Medicine (Review). 376 (10): 957–70. doi:10.1056/NEJMra1505557. PMID 28273019. S2CID 43867408.
- Amherd-Hoekstra A, Näher H, Lorenz HM, Enk AH (May 2010). "Psoriatic arthritis: a review". Journal of the German Society of Dermatology. 8 (5): 332–9. doi:10.1111/j.1610-0387.2009.07334.x. PMID 20015187. S2CID 25484225.
- "Psoriatic Arthritis". Arthritis Action. Archived from the original on 27 January 2016. Retrieved 12 August 2015.
- Davidson, Stanley, Davidson's principles and practice of medicine, Churchill Livingstone/Elsevier, p. 1096, 2010. ISBN 9780702030857. Accessed 2016-11-12.
- Farragher TM, Lunt M, Plant D, Bunn DK, Barton A, Symmons DP (May 2010). "Benefit of early treatment in inflammatory polyarthritis patients with anti-cyclic citrullinated peptide antibodies versus those without antibodies". Ann. Rheum. Dis. 62 (5): 664–75. doi:10.1002/acr.20207. PMC 2962800. PMID 20461787.
- Liu Y, Helms C, Liao W, et al. (March 2008). Leal SM (ed.). "A genome-wide association study of psoriasis and psoriatic arthritis identifies new disease loci". PLOS Genet. 4 (3): e1000041. doi:10.1371/journal.pgen.1000041. PMC 2274885. PMID 18369459.

- Rahman P, Elder JT (March 2005). "Genetic epidemiology of psoriasis and psoriatic arthritis". Ann. Rheum. Dis. 64 (Suppl 2): ii37–9, discussion ii40–1. doi:10.1136/ard.2004.030775. PMC 1766868. PMID 15708933.
- "Psoriatic Arthritis". The Johns Hopkins University School of Medicine and the Johns Hopkins Arthritis Center. Retrieved 2011-05-04.
- mayoclinic.org - Psoriatic arthritis
- nhs.uk
- versusarthritis.org
Psoriatic Arthritis: Causes and Manifestations of Psoriasis with Joint Infection
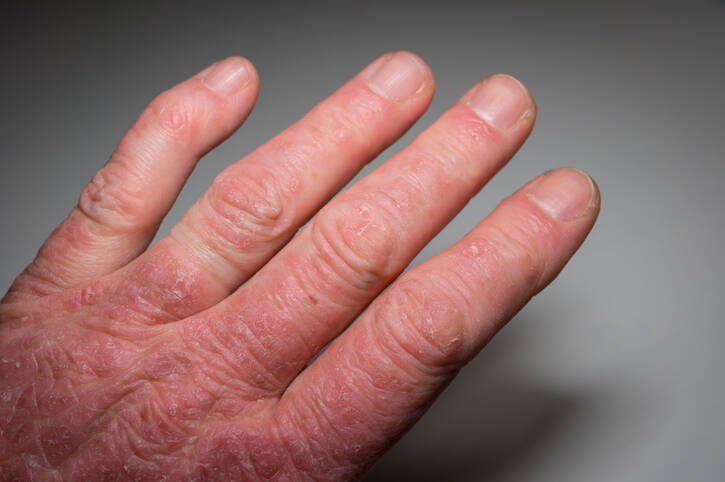
Photo source: Getty images
Most common symptoms
- Malaise
- Abdominal Pain
- Joint Pain
- Limb pain
- Flank Pain
- Deformed nails
- Depression - depressed mood
- Brittle nails - onychoschizia
- Swelling of the limbs
- The Island
- Swollen fingers
- Eye irritation
- Deepened nails
- Back Pain
- Bone thinning
- Dry skin
- Muscle weakness
- Itchy skin
- Itchy scalp
- Cutting the eye
- Fatigue
- Anxiety
- High blood pressure
- Reddened skin
- Redness of the conjunctivae
- Blurred vision
- Deterioration of vision
Show more symptoms ᐯ
Treatment of psoriatic arthritis: medications and other therapies
Show morePsoriatic arthritis is treated by
Other names
Arthritis psoriatica, arthropathic psoriasis, psoriatic arthropathy










