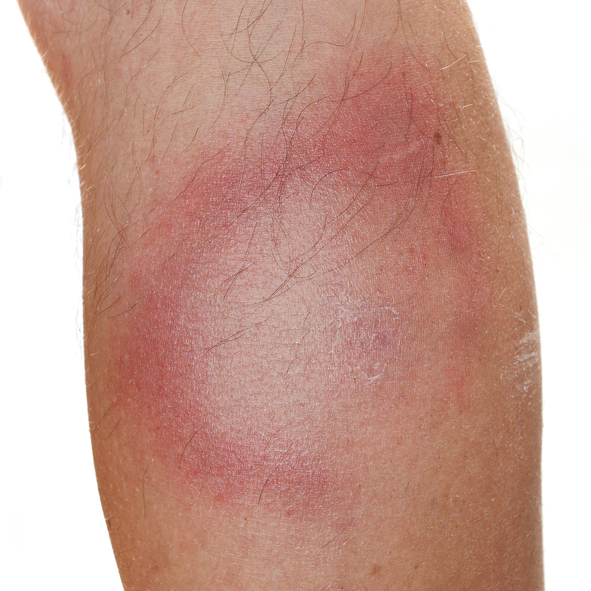
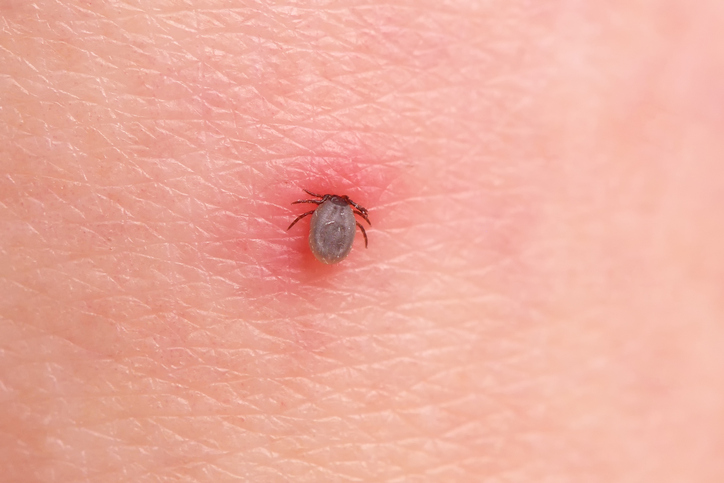
- "Signs and Symptoms of Lyme Disease". cdc.gov.
- "Lyme disease - Symptoms and causes". Mayo Clinic.
- Shapiro ED (May 2014). "Clinical practice. Lyme disease" (PDF). The New England Journal of Medicine. 370 (18): 1724–1731.
- "Lyme Disease Diagnosis and Testing". cdc.gov. 10 January 2013.
- Kugeler KJ, Schwartz AM, Delorey MJ, Mead PS, Hinckley AF (February 2021). "Estimating the Frequency of Lyme Disease Diagnoses, United States, 2010-2018". Emerging Infectious Diseases. 27 (2): 616–619.
- Wolcott KA, Margos G, Fingerle V, Becker NS (September 2021). "Host association of Borrelia burgdorferi sensu lato: A review". Ticks and Tick-Borne Diseases. 12 (5): 101766.
- Aucott J, Morrison C, Munoz B, Rowe PC, Schwarzwalder A, West SK (June 2009). "Diagnostic challenges of early Lyme disease: lessons from a community case series". BMC Infectious Diseases. National Library of Medicine. 9: 79.
- Aucott JN (June 2015). "Posttreatment Lyme disease syndrome". Infectious Disease Clinics of North America. 29 (2): 309–323.
- Johnson RC (1996). "Borrelia". In Baron S, et al. (eds.). Baron's Medical Microbiology (4th ed.). Univ of Texas Medical Branch. ISBN 978-0-9631172-1-2. PMID 21413339.
- "Lyme disease transmission". cdc.gov.
- Steere AC, Strle F, Wormser GP, Hu LT, Branda JA, Hovius JW, et al. (December 2016). "Lyme borreliosis". Nature Reviews. Disease Primers. 2: 16090.
- "Lyme borreliosis" (PDF).
- Pritt BS, Mead PS, Johnson DK, Neitzel DF, Respicio-Kingry LB, Davis JP, et al. (May 2016). "Identification of a novel pathogenic Borrelia species causing Lyme borreliosis with unusually high spirochaetaemia: a descriptive study". The Lancet. Infectious Diseases. 16 (5): 556–564.
Lyme disease: How does transmission occur and how does it manifest? + Treatment
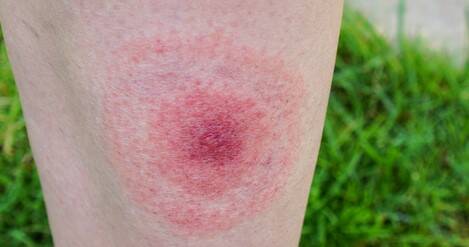
Photo source: Getty images
Most common symptoms
- Muscle Pain
- Malaise
- Headache
- Joint Pain
- Limb pain
- Skin pain
- Nerve pain
- Eye Pain
- Back Pain
- Sensitivity to light
- Fever
- Double vision
- Tinnitus
- Bone Pain
- Rash
- Dementia
- Nausea
- Defence
- The Island
- Falling eyelids
- Tingling
- Eye irritation
- Buds
- Muscle weakness
- Itchy skin
- Fatigue
- Vomiting
- Reddened skin
- Redness of the conjunctivae
- Deterioration of vision
- Yellowish skin
- Enlarged lymph nodes
- Increased body temperature
Show more symptoms ᐯ
Treatment of Lyme disease: drugs, antibiotics
Show more