- Rapini RP, Bolognia JL, Jorizzo JL (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. p. 1135. ISBN 978-1-4160-2999-1.
- Westerberg DP, Voyack MJ (December 2013). "Onychomycosis: Current trends in diagnosis and treatment". American Family Physician. 88 (11): 762–70. PMID 24364524.
- "Onychomycosis – Dermatologic Disorders". Merck Manuals Professional Edition. February 2017. Retrieved 2 June 2018.
- Rodgers P, Bassler M (February 2001). "Treating onychomycosis". American Family Physician. 63 (4): 663–72, 677–8. PMID 11237081.
- Kreijkamp-Kaspers S, Hawke K, Guo L, Kerin G, Bell-Syer SE, Magin P, et al. (July 2017). "Oral antifungal medication for toenail onychomycosis". The Cochrane Database of Systematic Reviews. 2017 (7): CD010031. doi:10.1002/14651858.CD010031.pub2. PMC 6483327. PMID 28707751.
- Rigopoulos D, Elewski B, Richert B (2018). Onychomycosis: Diagnosis and Effective Management. John Wiley & Sons. ISBN 9781119226505.
- Liddell, Henry George; Scott, Robert; A Greek–English Lexicon at the Perseus Project.
- NHS Choices: Symptoms of fungal nail infection
- Mayo clinic: Nail fungus
- Onychomycosis at eMedicine
Nail Mycosis, Fungal Infection of Nails and Toenails: Manifestations And Removal
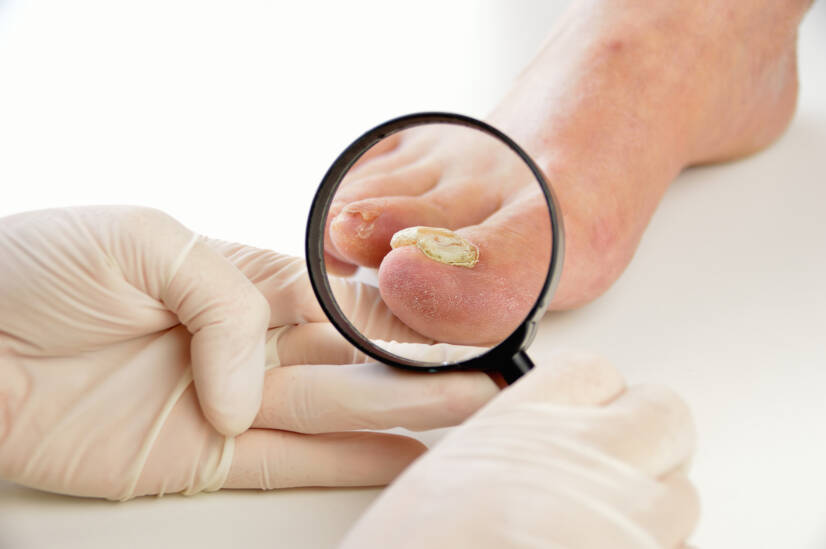
Fungi on feet and (toe)nails is one of the most common skin problems. Lifestyle choices and a suitable environment for the multiplication of pathogens exacerbate the infection. It is chronic and has a negative impact on the physical and mental well-being. The condition is also knon as mycosis, onychomycosis, dermatophytic onychomycosis, and tinea unguium.
Most common symptoms
- Skin pain
- Leg Pain
- Heel Pain
- Deformed nails
- Rash
- Brittle nails - onychoschizia
- Wetting of the skin
- Sweating
- Strokes on the nails
- Swollen fingers
- Blisters
- White patches on the skin
- Deepened nails
- Buds
- Dry skin
- Itchy skin
- Reddened skin
Characteristics
FAQ:
Is nail mycosis responsible for the thickening of the nails?
How can nail fungus be removed?
Will applying vinegar, garlic, or colloidal silver on the nails do anything? WHat about laser treatment for onychomicosis?
Fungal diseases are among the most common skin problems. Fungi can cause various difficulties that make life very uncomfortable. However, they do not only affect the surface of the skin or nails, but deeper parts of the skin, too. In some cases, they might be considered organ diseases.
Foot and nail fungus are becoming an increasingly common problem. This is because the conditions we create for them is just right. Skin problems due to fungal diseases will be discussed in the rest of the article.
On Fungi - A Brief Overview
To date, there are approximately 150,000 species of known fungi. Of these, about 180 species are dangerous to humans. Fungi are cellular plants. They have a cell wall and a nucleus. Since they do not have chlorophyll, they need organic matter and oxygen to survive, grow and reproduce.
In addition, it is important for fungi to be in a suitable environment. For example, higher humidity, alkaline environment and temperature are important factors. The ideal temperature for their growth and multiplication is around 36.7 °C. This is where their frequent presence, especially on the surfaces of the feet and toenails, comes in.
We have created a perfect environment inside our footwear and the right composition of artificial clothing fibres, such as socks. Fungi love sports and group activities. Also, reduced immunity and associated diseases, such as diabetes, contribute to their multiplication.
The classification of fungi is bsed on several properties. For example, the structure of fibrous fungi, their hyphae, and unicellular yeasts. There are geophilic fungi transmitted to humans from the soil, zoophilic fungi from animals, and anthropophilic fungi spreading from person to person.
Based on another method, fungi are divided into those which occur only when the conditions are right for them to start multiplying. Those are also referred to as saprophytic. The second group includes pathogenic fungi. They will become a nusiance at all times.
There are Different Types of Mycoses
Fungi can cause a wide variety of diseases. However, a fungal disease can promote the presence of another underlying disease, such as diabetes or cancer. Fungi fall into three main categories.
There are three categories of fungal skin diseases:
- dermatophytosis
- cutaneous candidiasis
- skin diseases associated with Malassezia
Dermatophytosis, also known as tinea and ringworm. These diseases are further classified according to the site they affect, such as tinea pedis. This form of fungi affects the foot. This group of diseases is also known as athlete's foot or moccasin foot. To make it even more confusing, there are even more classifications.
Table: Detailed Classificatiom of Skin Mycoses
| Tinea | Candidiasis | Malassezia |
|
a.k.a dermatophytosis the technical term indicates the site of occurrence |
Most common pathogens:
|
The disease is mostly caused by Malassezia furfur
In addition, the following species are found on healthy skin:
|
| Tinea pedis the most common form of disease it mainly affects the foot and the area between the toes starting at 18 years of age sports activities have a high impact on its occurrence It is further divided into:
| Candidosis mucosea oris the most common fungal infection in newborns and children under 1 year of age also known as:
| Pityriasis versicolor mainly in adults in places with a higher incidence of sebaceous glands |
| Tinea unguium a.k.a. onychomycosis, which is a broader concept that includes other diseases a fungal infection of the nail most often due to the chronic occurrence of tinea pedis tehre are 4 types:
| Candidosis intertriginosa occurs in the areas between the fingers in elderly and obese women on the chest - scabs in young children such as some types of diaper dermatitis | Malassezia folliculitis rare and chronic disease mainly affects women aged 25-35 |
| Tinea corporis affects the chest it often occurs when the immune system is weakened or after treatment with corticosteroids | Vulvovaginitis candidosa is a disease of the female genitalia in most cases as an acute infection in some cases as a chronic and relapsing form that is difficult to treat | |
| Tinea inguinalis affects the groin area and the thighs especially in young males contributes to her tight and airtight clothing | Balanitis candidosa is a disease of the glans especially after sexual intercourse | |
| Tinea capitis affects the scalp, the hairy part most often affects children after transmission from an animal the commonest causative agent is Microsporum canis | Candida onychomycosis as a result of paronychia | |
| Tinea faciei affects part of the face | Candida paronychium is a disorder of the nail folds | |
| Tinea manus most often transferred from the feet rare form | chronic mucocutaneous candidiasis usually as a result of an immune and endocrine disorder it often starts in childhood |
TIP: Learn more in the articles Skin pain and Nail deformities.
Table: Classification of Mycosis Bases on Clinical Evaluation
| Name | Description |
| Superficial mycosis | affects the epidermis, ie the skin, the upper part of the skin dermatomycosis affects the stratum corneum, which is the upper part of the skin and thus the first barrier to the outside world |
| Deep mycosis | affects the skin as well as subcutaneous structures |
| Systemic mycosis | affects body systems and organs |
Foot and nail fungus make us think about...
Molds on the feet and nails cause wrinkles on many people. They are among the most common skin problems in the human population. In case of difficulties, it is necessary to think of diseases which are referred to as Tinea pedis, Tinea unguium or even onychomycosis.
Tinea pedis
The name itself already indicates that it is a disease of the foot. It is classified as a dermatophytosis and is the most common fungal disease. It can affect up to 50% of the population. It is most often caused by T. rubrum, T. interdigitalis, E. floccosum, but also by Candida or Trichosporon.
Fungal disease is further divided based on the site of affliction, i.e. plantar (soles) and interdigital (between toes, fingers) tinea. The disease is often chronic and recurrent. People with this problem also have issues with excessive sweating. That is why it is important to prevent the disease, such as by wearing appropriate footwear or socks that breathe and are made of natural fibres.
Tinea unguium, or nail fungus
It is named after a fungal nail infection. This form most often develops from tinea pedis. Only in very rare cases does a primary nail disease occur. Tinea unguium falls into the broader term onychomycosis. Thus, tinea is a form of dermatophytosis.
Onychomycosis is an indicator of a variety of pathogens. It is most often caused by dermatophytes and less often by fungi and other pathogens. In up to 50 percent of cases, it is the result of a nail deformity. It mainly affects adults, especially the toenails.
Risk factors include:
- sex, with men being more likely to be affected
- age, affects up to 60% of the elderly
- employment, fungal diseases of the hands, such as hands being soaked for a long time (cleaners, dishwashers, etc.)
- climate
- travelling
- sports activities and hobbies
- unsuitable footwear, closed and non-breathable footwear
- poor level of hygiene, poor nail hygiene
- nail injuries
- medicine, such as antibiotics, immunosuppressants
- associated diseases
- diabetes
- weakened immunity
- chronic venous insufficiency of the legs, worsened blood flow to the legs
- psoriasis
Toenails are affected 7 times more often
Of course, fungi are not the only cause of these issues. Differential diagnosis is important to determine a correct diagnosis. Although about 50% of nail diseases are caused by fungi, there may be other problems, such as nail psoriasis, the commonly known ingrown nail (unguis incarnatus) and others.
Causes
Today's modern way of life contributes to these issues. Fungi, molds, yeasts, and thus mycoses in general thrive in a suitable environment. This represents higher humidity or temperature. Mass sports and people staying in larger numbers, for example at swimming pools, further help fungi to multiply.
Another example is today's footwear and clothing which ismade of artificial fibres. This type of clothing does not breathe, it creates a humid environment, and thus contributes to the multiplication of pathogens. The worst combination is garment which is non-breathable and tight.
Of course, there are also some types of jobs where employees are exposed to mycosese, especially when they are required to wear tight safety footwear throughout working hours, which increases sweating.
Onychomycosis is most often caused by:
Trichophyton rubrum 65 - 90 %
Trichophyton interdigitale 5 - 15 %
Scopulariopsis brevicularis 2 - 8 %
Aspergillus 2 - 8 %
Fusarium 1 - 3 %
Epidermophyton floccosum 1 %
less frequently by Candida albicans and tropicalis
A special group are systemic diseases that are associated with mycosis. These diseases are mainly related to the skin. They reach it superficially or even deeply. However, they can also damage subcutaneous structures.
Fungal disease can also cause problems with the body's systems and organs. As is the case, for example, in women with candidiasis of vulva and vagina. Another case is aspergillosis and other invasive fungal infections.
The presence of the underlying disease also contributes to the development of mycosis. People with diabetes, endocrine disorders, but also with weakened immunity are more prone. AIDS or cancer is a serious risk.
The most common source of infection is an infected person.
Common places of transmission are mainly social spaces where people move about barefoot.
Swimming pools, shared showers.
Transmission occurs due to a skin injury, mucous membranes, and by touch.
Medicications, too, have an effect. Fungal diseases commonly occur after an antibiotic treatment, but also during treatment with corticosteroids, cytostatics and immunospuppressives which suppress human immunity, especially after transplantation.
Learn more in the following articles:
What should we worry about in the summer?
Swimming in lakes and pools
Alcohol and bodies with water
Symptoms
Infection of the skin on the toes and around the nails results in difficulties, such as unbearable itching or even burning. However, pain may not always be present.
In some cases, the condistion may be associated with soaked skin, or even blisters.
Other times, the skin is dry and cracked, especially on the soles or heels.
It is pale.
The feet have an odour.
As the infection spreads to the nail, the skin beneath it starts to change. There is increased cornification (production of keratin), i.e. hyperkeratosis. The nail surface is still undamaged, but it is somewhat elevated.
The nail turns yellow. Later on, the nail wall and nail bed may also be affected. The skin above the nail is red and swollen.
Table: Symptoms occurring with mycosis of the feet and nails
| Disease | Type | Symptoms |
| Tinea pedis | Interdigital | most often fungi on the feet, in interdigital area IV white and soaked skin itching after the acute phase, the skin is peeling |
| Hyperkeratotic |
most often on the foot, edges of the foot and heel red rough sites peeling skin no subjective difficulties chronic | |
| Vesiculobullous |
strong itching rash especially on the sole alternating oiutbreaks | |
| Onychomycosis a.k.a. Tinea unguium | mostly Trichophyton rubrum, T. interdigitale, Epidermophyton floccosum and yeast | Nail fungi are most common as an extension, skin mycosis |
| distal subungual |
the most common form, affects the nails of the hands but especially the feet on the "free" edge of the nail advances to the nail skin wall hyperkeratosis, i.e. excessive skin keratinization nail thickening nail deformity nail discolouration to yellow | |
| proximal subungual | a rare form starts at the nail wall on finger nails and toenails in approximately equal proportions excessive skin keratinization white spots on the nails destruction of the nail plate | |
| white superficial | most often with reduced immunity especially on the toenails matt white delimited bearings rough appearance of the nail a large area of the nail can also be affected | |
| endonyx | rare occurrence nail plate involvement whitish nail | |
| total dystrophic onychomycosis | total nail damage in a chronic disease course until the final loss of the nail |
Diagnostics
A mycological examination will determine the type of fungal disease. A microscopic fungal test (KOH) and culture are carried out. It is important to identify the causative agent and the pathogen that caused the problem. This is especially important in antifungal treatment, as not all medications affect all fungi.
Therefore, treatment should not be based solely on a clinical evaluation of visible symptoms. Nail sampling is also performed. These samples are taken before the start of treatment, but also after at least 2-4 weeks. A follow-up examination is performed after 3-6 months.
A nail sample is obtained by curettage. Staining is used to prepare the sample for a microscopic examination. If the examination is negative, a histopathological examination of the nail sample may be performed. Nail biopsy is an important procedure to eliminate nail psoriasis.
Course
One of the first symptoms may be an unpleasant itching. Subsequently, the skin can be moist, soaked, macerated. This acute stage goes through, the skin is dry and peeling. Skin scales may be present for a long time. The chronic form may be painless, or does not itch at all.
The food fungal poison aflatoxin, which is the cause of liver cancer, is dangerous.
The skin may be red, in some cases swollen. This is especially the case with an infection that is located at the site of the skin nail wall. In the nail area, the skin is excessively keratinised, which raises the nail plate. The damaged nail changes its colour and may turn yellow or brown. The nail may have white spots or be entirely white.
At first, the nail is rough, and later on, it changes its shape. Total dystrophic onychomycosis is characterized by the fact that the nail is totally damaged and breaks off. This condition is typical of a long-lasting fungal disease.
Early diagnosis and identification of the pathogen are important to plan the treatment. In some cases, treatment is lengthy. The disease is chronic or recurrent, i.e. it keeps returning.
Mycosis prevention is very importanct
Prevention is important not only prior to the onset of the disease, but also after the condition has healed. Fungi need a suitable environment for their growth, multiplication and expansion. They also need dampness and warmth. Insufficient hygiene, ill-fitting shoes and clothes or underwear also have a negative effect.
It might be good to think about having your own shoes and towel in case you might want to use shared sanitary facilities. After washing, it is necessary to thoroughly dry the skin, even in the areas between the fingers. It is also important to regularly disinfect your footwear, especially for sports activities, or if the footwear does not breathe.
Fungi are concentrated in places, such as:
- outdoor swimming venues
- thermal baths
- indoor swimming pools
- areas around the pool
- indoor/outdoor sports areas
- indoor sports venues
- locker rooms
- shared showers and communal baths
- všade tam, kde chodia ľudia bosí
Dermatophyte spores survive for weeks, months or years, for example in footwear, underwear, carpets, but also on nail files or in shoes in shoe stores.
Breathable clothes or cotton socks are helpful. Being barefoot helps the foot breathe. For people who suffer from increased sweating, there are antihydrotic agents that reduce sweating. Early treatment is very important in case of difficulties. Initially, an over-the-counter medication could be enough.
How it is treated: Fungal Infection of Nails and Toenails
How is nail mycosis treated? Medication and surgery
Show moreVideo about fungal diseases
Fungal Infection of Nails and Toenails is treated by
Other names
Interesting resources
Related










