- ncbi.nlm.nih.gov - Maturity Onset Diabetes in the Young
- mayoclinic.org - Latent autoimmune diabetes in adults (LADA): What is it?
- healthline.com - New Drug Treatment Options for Diabetes
- pubmed.ncbi.nlm.nih.gov - Insulin therapy in type 2 diabetes
- pubmed.ncbi.nlm.nih.gov - Type 2 diabetes: the role of insulin
Diabetes: Causes, Symptoms, Complications
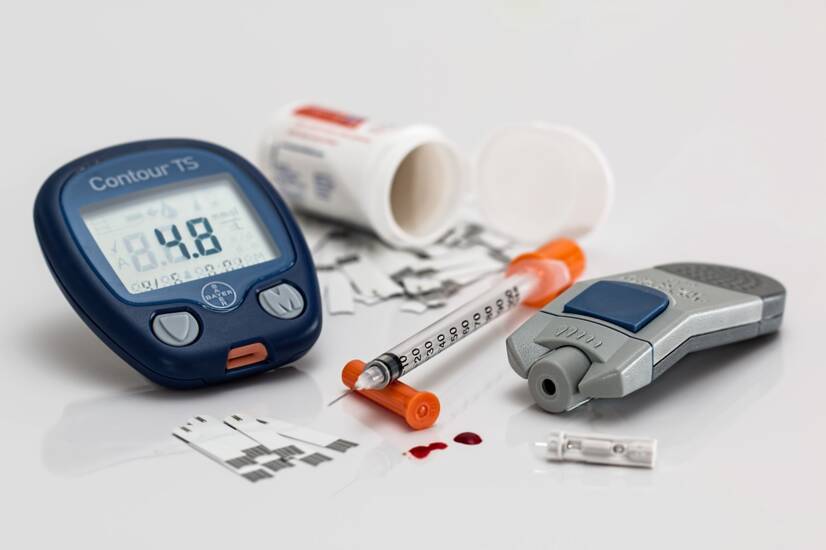
Diabetes is the most common metabolic disorder today. Elevated blood sugar, i.e. hyperglycaemia, has various causes and consequences.
Most common symptoms
- Acetone Breath
- Malaise
- Loss of pubic hair
- Leg Pain
- Frequent urination
- Frequent urge to urinate
- Sugar in urine
- Diarrhoea
- Indigestion
- Nausea
- The Island
- Blindness in one eye
- Tingling
- Eye irritation
- Slow wound healing
- Erectile dysfunction
- Memory disorders
- Disorders of consciousness
- Mood disorders
- Buds
- Blindness
- Cold extremities
- Muscle weakness
- Itchy skin
- Itchy scalp
- Tremor
- Fatigue
- Vomiting
- High blood pressure
- Reddened skin
- Blurred vision
- Deterioration of vision
- Increased appetite
- Increased blood sugar levels
Characteristics
Chronic complications of diabetes include serious diseases such as diabetic retinopathy, nephropathy, neuropathy, and diabetic foot, which often results in an amputation.
These complications are a consequence of untreated diabetes.
The basic principle of minimising the progression of chronic complications of diabetes is to maintain normal glycaemic levels, reduce weight and try to influence other cardiovascular risk factors such as high blood pressure and smoking.
Diabetes is the lay term for a common metabolic disease called Diabetes mellitus.
The disease is characterised by elevated blood glucose levels, called hyperglycaemia. Hyperglycaemia can have various causes and a number of consequences.
Hyperglycaemia occurs when the glucose we take in from food is not transferred from the blood into the cells, where it is used as the main source of energy for life. The glucose remains in the so-called extracellular space, i.e. in the blood.
The most important sources of glucose are starch, sucrose and other carbohydrates. The body also has its own stores of glucose that it can use efficiently in the event of starvation.
Glycogen, which is stored in the liver, is the main source of glucose. The process by which glycogen is broken down into glucose is called glycogenolysis. It takes place in liver cells called hepatocytes.
Another way the body can help itself in the event of a carbohydrate deficiency is through a process called gluconeogenesis.
It is the "production" of glucose from non-saccharide compounds, e.g. proteins. It occurs in the liver and kidneys. This way, the body can produce up to 100 grams of glucose.
In periods of extreme exhaustion of the organism, e.g. during severe infections, the production is increased to 400 grams per day.
The body uses the glucose from the diet, but after 5 hours of fasting it starts to convert its own sources, i.e. glycogen and non-carbohydrate sources, into glucose.
The biggest consumer of glucose is the brain. It needs 100 to 150 grams of glucose a day.
Other glucose-hungry consumers include the muscles and fat cells. They make up to half of all cells in the body. Glucose enters the cells via glucose transporters (GLUT).
The glucose transporters that carry glucose into muscle and fat cells are called GLUT4. These GLUT4 transporters need insulin in order to function. Other glucose transporters are insulin-independent and can function without insulin.
It follows that at least half of our body's cells, muscle and fat cells, do not receive their energy supply in the form of glucose if an adequate amount of insulin is not present in the blood or if its effect is inadequate.
Unused glucose remains circulating in the blood and increases to a higher the glycaemic level every time we eat.
Glucose is an osmotically active substance, which means it draws water. The kidneys react to the increased osmolality of the body by increased water excretion, which causes increased urination, dehydration and excessive thirst.
The high amount of glucose available in the blood also has an impact on other building blocks, such as proteins. They undergo glycation to form so-called advanced glycation end products, or AGEs. These substances are difficult to dissolve as not even enzymes cannot break them down.
Since there is too much of it and the body cannot use it, these products start to be stored in various organs, e.g. in the kidneys.
Advanced glycation end products (AGEs) are the reason for late chronic complications of diabetes.
Causes
- Type 1 diabetes mellitus
- Type 2 diabetes mellitus
- Other types of diabetes
Type 1 diabetes mellitus
Type 1 diabetes is a type of diabetes characterised by a total lack of insulin.
About 10% of all diabetics have type 1 diabetes mellitus.
Insulin is a hormone produced by the pancreas. It is secreted by the beta-cells of the islets of Langerhans. If these cells are damaged or destroyed, e.g. by an autoimmune process, they are unable to produce and secrete insulin.
A loss of at least 80-90% of the islets of Langerhans will lead to the development of diabetes mellitus. With such a small number of beta cells remaining, the body is no longer able to produce enough insulin, and the symptoms of diabetes become fully apparent.
An autoimmune inflammation of the islets of Langerhans is called insulitis. The principle of the autoimmune reaction is the existing genetic predisposition (presence of HLA genes DR3 and DR4) and a trigger factor, e.g. viral infection, Coxackie B, parotitis virus, influenza, measles, or other external stress risk factors.
An autoimmune inflammation is mediated by immune cells:
- lymphocytes, specifically a population of Th-1 lymphocytes with features of CD4+ and CD8+
- macrophages
Besides cellular immunity, humoral immunity is also involved in the autoimmune process, which gradually produces diabetes-associated autoantibodies.
They do not have a direct role in beta-cell destruction, but are used in diagnostics to monitor the activity of autoimmune inflammation.
Type 1 diabetes mellitus is a lifelong disease that is usually diagnosed in childhood, most often by the age of 4. The younger the age at the onset of autoimmune destruction, the faster the whole process and the more rapid the manifestation of diabetes.
Type 2 diabetes mellitus
Type 2 diabetes mellitus is characterised by insulin resistance or relative insulin deficiency.
In this type of diabetes, a sufficient amount of insulin is present in the blood, but the cells do not respond to it, which is why glucose is not transferred into the cell.
In the 1960s, insulin resistance was defined as a condition in which a normal concentration of insulin results in a reduced biological response of the cells.
This discovery was made by Berson and Yallow, two scientists who had been radiolabelling the insulin molecule and studying its biological behaviour in the human body.
Other types of diabetes
- Endocrine diabetes: hyperglycaemia also occurs in some endocrine diseases, e.g. thyroid disease, Cushing's syndrome, acromegaly, pheochromocytoma, hyperaldosteronism, somatinostatinoma, and glucagonoma.
- Diabetes in pancreatic diseases: Diseases in which beta-cells are damaged, e.g. chronic pancreatitis, pancreatic carcinoma and cystic fibrosis.
- MODY: Maturity Onset Diabetes in the Young is a genetic disorder of beta-cells leads to diabetes comparable in cause to type 1 diabetes (i.e. total insulin deficiency), but does not become clinically apparent until adulthood, around the age of 30.
- LADA: Latent autoimmune diabetes in adults is diabetes mediated by autoimmunity, similar to type 1 diabetes mellitus, but occurs later in life, hence the designation "latent". It is also associated with total insulin deficiency, but the disease progresses much slower, so there is no need to initiate insulin treatment for several years after diagnosis.
- Gestational diabetes: this type of diabetes is similar to type 2 diabetes. Whether insulin secretion is normal or increased, the blood screen will show hyperglycemia, which is caused by insulin resistance of the cells. Pregnancy and placental hormones, especially cortisol and the so-called human placental lactogen, are the cause of this type of diabetes. The peak secretion of these hormones is from approximately the beginning of the second trimester. Gestational diabetes affects approximately 3% of pregnant women and the incidence of this type of diabetes is increasing, as is the incidence of type 2 diabetes.
- Drug-induced diabetes: certain medications can induce secondary diabetes, e.g. glucocorticoids, thiazide diuretics, diazoxide, beta-adrenolytics, interferons, etc.
Symptoms
In type 1 diabetes, symptoms usually appear more quickly and are more severe.
Symptoms of diabetes include:
- increased thirst
- frequent urination
- extreme hunger
- unexplained weight loss
- ketones in the urine (ketones are a by-product of protein breakdown that occurs when there is a lack of available insulin)
- fatigue
- irrritability
- blurred vision
- poorly healing wounds
- common infections such as gum or skin infections and vaginal infections
Symptoms of acute and chronic complications of hyperglycemia
Acute complications of diabetes
- Diabetic ketoacidosis - an acute life-threatening complication of type 1 diabetes where the patient becomes unconscious or even comatose. It is caused by an absolute deficiency in insulin secretion, which induces hyperglycaemia, hyperosmolality, dehydration, an increased production of ketone bodies, which leads to ketoacidosis with acidification of the body's internal environment to pH 6.8, which is fatal. The treatment is insulin administration (injection), rehydration and potassium supplementation.
- Hyperosmolar hyperglycemic state (HHS) - a typical complication of type 2 diabetes, where insulin is secreted without the production of ketone bodies, but since blood glucose rises, there will be dehydration and increased fluid loss.
The condition progresses slowly, sometimes over days or weeks. In the advanced state, patients are brought to the hospital in a hypovolemic shock, with failing kidneys and brain swelling.
Treatment consists mainly of rehydration and insulin administration. Although treatment management has improved, about 10% of patients die.
- Hypoglycaemic coma - occurs after an overdose of insulin or certain antidiabetic drugs.
Manifestations of hypoglycemia:
- increased sweating,
- accelerated heart rate,
- limb tremors,
- inability to concentrate
- unbearable hunger
- confusion
- coma
Treatment: glucose injections.
Learn more:
- Blood sugar levels: Normal levels and Hyper/Hypoglycemia
- Hypoglycemia: Manifestations of low blood sugar, complications
- Hyperglycaemia: Manifestations, Treatment
- Measuring your Blood Pressure, Pulse, Breathing, and Glycemia at home
Chronic complications of diabetes
- Diabetic nephropathy - chronic kidney damage that causes AGEs and high blood pressure. In the first stage, the kidneys pass the smallest proteins into the urine, a condition called microalbuminuria. As the disease progresses, larger amounts of protein are excreted into the urine, leading to nephropathy, which ends in kidney failure.
- Diabetic retinopathy - the proliferative form of the disease causes vision impairment and blindness.
- Diabetic neuropathy - has many forms, e.g. sensory neuropathy, impaired motor functions, pain, and autonomic neuropathy. Neuropathy is frequently the first symptom of diabetes, but it can remain asymptomatic for years.
- Diabetic foot - it is a complication of worsening diabetic neuropathy, reduced sensation in the feet, limited microcirculation in combination with chronic injuries, for example when wearing inappropriate size shoes, poorly healing inflamed wounds, ulcers, phlegmon, foot gangrene.
Learn more:
Diagnostics
The blood test shows an elevated glucose level, a condition called hyperglycaemia.
Normal fasting glycemia ranges from 3.3 to 5.6 mmol/l.
A random glucose test measured at any time of the day should not show a value higher than 7.8 mmol/l.
When the random glucose level is above 11.1 mmol/l or a repeated fasting glucose level is above 7.0 mmol/l, the diagnosis is diabetes.
Of the values are borderline, an oral glucose tolerance test (OGTT) is performed, where the patient is given a sweet water solution and 75 grams of glucose to drink. Glycaemia is then assessed after 120 minutes.
If the glucose level is above 11.1 mmol/l, the diagnosis is diabetes. With values below 7.8 mmol/l, diabetes can be excluded, but the patient can be monitored for some time.
Borderline values between 7.8 - 11.1 mmol/l are a sign of impaired glucose tolerance.
In addition to glycaemia, it is also advisable to monitor glycated haemoglobin values as part of regular diabetic check-ups, which is a better indicator of the long-term compensation of diabetes.
Glycolated hemoglobin is the final product of hemoglobin with a glucose molecule attached. The binding of glucose to hemoglobin is a process that occurs periodically throughout life, but is dependent on glycemic values.
With prolonged high blood glucose concentrations, the exposure of hemoglobin to glucose molecules is prolonged, which promotes cross-linking.
This way blood glucose levels over the last 6-8 weeks ocan be checked. This is done because after this time period the red blood cells, i.e. haemoglobin, are replaced.
Course
Hyperglycaemia in children will frquently present with severe abdominal pain, which may mimic a sudden abdominal episode, e.g. appendicitis or acute gastritis.
When type 1 diabetes is diagnosed, it is a lifelong disease that requires insulin administration.
Type 2 diabetes is diagnosed in adulthood, most commonly after the age of 50. The rate of manifestation depends on hereditary and environmental factors such as lifestyle and diet.
It is not uncommon for type 2 diabetes to occur as a hidden disease, which is diagnosed only when complications appear, e.g. when unpleasant diabetic neuropathy, nephropathy, or visual impairment in diabetic retinopathy occurs.
The basic principle of slowing down the progression of chronic complications of diabetes is done in order to maintain normal glycaemic levels, reduce weight and try to influence other cardiovascular risk factors such as high blood pressure or smoking.
This article was made possible thanks to the support of Hemp Point CBD Slovakia.
How it is treated: Diabetes
Liečba Diabetes Mellitus: Lieky, inzulín, diéta. Dá sa vyliečiť?
Show moreDiabetes is treated by
Other names
Interesting resources
Related










