- my.clevelandclinic.org - Adult Jaundice
- medicinenet.com - Jaundice in Adults (Hyperbilirubinemia)
- niddk.nih.gov - What Is Viral Hepatitis?
- medicalnewstoday.com - Everything you need to know about jaundice
- my.clevelandclinic.org - Gilbert's Syndrome
Jaundice: Causes, Symptoms, Treatment
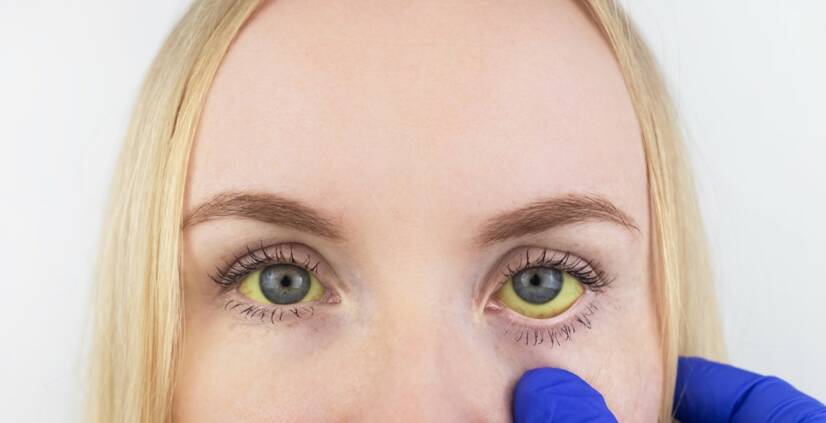
Jaundice (icterus) is a yellowish discoloration of the tissues by an increased concentration of bilirubin: the bile pigment. Small increases (subicterus) can be seen on the sclerae (whites of the eyes) and soft palate. Jaundice is not a disease in itself, jaundice is a symptom of a disease.
Most common symptoms
- Muscle Pain
- Malaise
- Right Flank Pain
- Abdominal Pain
- Headache
- Joint Pain
- Limb pain
- Fever
- Diarrhoea
- Stool with blood - blood in the stool
- Indigestion
- Nausea
- Swelling of the limbs
- The Island
- Light stool
- Itchy skin
- Dark urine
- Fatigue
- Water in the abdomen
- Yellow whites of the eyes
- Winterreise
- Yellowish skin
- Confusion
- Liver enlargement
- Increased body temperature
Characteristics
Elevated bilirubin in the blood that is the cause of jaundice is called hyperbilirubinemia.
The normal level of bilirubin is between 2.0 - 17 mmol/l, we usually speak of hyperbilirubinemia if the level is higher than 20 mmol/l.
Bilirubin is a normal breakdown product in the catabolism of heme, which is a component of hemoglobin, the red blood pigment, and is thus produced in the destruction of red blood cells.
Normally, bilirubin undergoes conjugation in the liver, making it water soluble. It is then excreted in the bile into the gastrointestinal tract, the majority being excreted in the faeces as urobilinogen and stercobilin (a product of the metabolic breakdown of urobilinogen).
Approximately 10% of urobilinogen is reabsorbed into the bloodstream and excreted by the kidneys.
Many babies are also born with high bilirubin, causing a condition called neonatal jaundice. This causes yellow-colored skin and eyes in babies.
This condition occurs because at birth the liver is often not yet fully able to process bilirubin. This is a temporary condition that usually corrects itself within a few weeks.
Causes
Prehepatic jaundice
In this type of jaundice, there is an increased production of unconjugated haemoglobin, which the liver is unable to process.
It is formed when red blood cells break down excessively and this causes unconjugated hyperbilirubinemia.
Liver damage is not present.
Hepatic jaundice
In hepatic or hepatocellular jaundice, we find liver cell dysfunction. The liver loses its ability to conjugate bilirubin, but in cases where cirrhosis also occurs there is also a degree of obstruction.
This leads to elevated both unconjugated and conjugated bilirubin in the blood, which is sometimes called a "mixed picture".
Posthepatic jaundice
Posthepatic jaundice means a disorder of bile outflow. Bilirubin that is not excreted is conjugated in the liver, thus resulting in conjugated hyperbilirubinemia.
Table: the most common types of jaundice
| Prehepatic icterus | Hepatic icterus | Posthepatic icterus |
|
|
|
Symptoms
In addition to the yellow discoloration of the skin and whites of the eyes, the patient may also suffer from other symptoms:
- light-coloured stool
- dark-coloured urine
- itching of the skin
- nausea and vomiting
- rectal bleeding
- diarrhea
- fever and chills
- fatigue
- weight loss
- loss of appetite
- confusion
- abdominal pain
- headache
- swollen feet/legs
- swelling and distention of the abdomen due to fluid accumulation (ascites)
Diagnostics
This is followed by blood sampling and assessment of liver parameters (ALT, AST, ALP, GGT).
More information also in the article:
What do liver tests reveal? What do elevated values mean?
Additionally, imaging modalities such as SONO/USG, ERCP, MRCP, CT, MRI (and others as needed and associated symptoms) are also performed.
Selected most common diseases causing jaundice
Viral hepatitis
Viral hepatitis is an infection that causes inflammation and damage to the liver. Several types of hepatitis are known; they are referred to as hepatitis A, B, C, D and E viruses.
Hepatitis A and hepatitis E are usually spread by contact with food or water that has been contaminated with an infected person's stool.
People can also get hepatitis E by eating undercooked pork, deer or shellfish.
Infected people have symptoms 2 to 7 weeks after contact with the virus. Patients with hepatitis A usually recover after a few weeks without treatment. In some cases, symptoms can last up to 6 months.
These symptoms may include:
- yellowish eyes and skin - jaundice
- dark yellow urine
- diarrhea
- fatigue
- fever
- joint pain
- loss of appetite
- nausea
- abdominal pain
- vomiting
In rare cases, hepatitis A can lead to liver failure. Liver failure due to hepatitis A is more common in adults over 50 years of age and in people who have other liver disease.
Hepatitis A is diagnosed by a blood test for IgM antibodies to hepatitis A in addition to the typical clinical picture.
How can I protect myself against viral hepatitis A? By getting vaccinated. After overcoming hepatitis A, the sick person also acquires lifelong immunity.
Hepatitis B
Acute hepatitis B is a short-term infection. Some people have symptoms that can last for several weeks. In some cases, symptoms last up to 6 months. Sometimes the body is able to fight off the infection and the virus goes away.
If the body is unable to fight the virus, the virus does not disappear and chronic hepatitis B infection occurs. Most healthy adults and children older than 5 years who have hepatitis B get better and do not develop chronic hepatitis B infection.
Chronic hepatitis B is a long-lasting infection. The chances of developing chronic hepatitis B are greater if the sick person is infected with the virus as a young child. About 90 percent of infants infected with hepatitis B will develop a chronic infection.
Approximately 25 to 50 percent of children infected between the ages of 1 and 5 years have chronic infections. However, only about 5 percent of people who first become infected as adults develop chronic hepatitis B.
Hepatitis B infection is more prevalent in some parts of the world, such as sub-Saharan Africa and parts of Asia, where 8 percent or more of the population is infected.
A person is more likely to get hepatitis B if they are born to a mother who has hepatitis B. The virus can spread from mother to baby during birth.
People are more likely to have hepatitis B if:
- They have HIV infection because hepatitis B and HIV are spread in a similar way.
- Have lived or had sex with someone who has hepatitis B.
- Have had more than one sexual partner in the last 6 months or have a history of a sexually transmitted disease.
- There are men who have sex with men.
- They are injecting drug users.
- They have a job in a profession such as healthcare where they have contact with blood, needles or bodily fluids at work.
- They live or work in a care facility for people with developmental disabilities.
- They have diabetes.
- They have hepatitis C.
- They live or travel frequently to parts of the world where hepatitis B is common.
- They were on kidney dialysis.
- They live or work in prison.
- They had a blood transfusion or organ transplant before the mid-1980s.
Acute complications of hepatitis B
In rare cases, acute hepatitis B can lead to acute liver failure, a condition in which the liver suddenly fails. People with acute liver failure may require a liver transplant.
Chronic complications of hepatitis B
Chronic hepatitis B can lead to:
- Cirrhosis - A condition in which scar tissue replaces healthy liver tissue and prevents your liver from functioning normally. Scar tissue also partially blocks blood flow through the liver. When cirrhosis worsens, the liver begins to fail.
- Liver failure, in which the liver is severely damaged and stops working. Liver failure is the final stage of liver disease. People with liver failure may require a liver transplant.
- Liver cancer: people with chronic hepatitis B have regular blood and ultrasound checks. Finding the cancer at an early stage increases the chance of curing the cancer.
Diagnosis of hepatitis B includes a medical history, physical examination, and blood tests to detect hepatitis B antibodies. An ultrasound examination is performed and in rare cases a liver biopsy is necessary.
Treatment for hepatitis B only begins in the chronic stage. Antiviral drugs (lamivudine, adefovir, entecavir) and peginterferon alfa-a2 (Pegasys) are taken.
How can I protect myself against viral hepatitis B?
The most effective protection against hepatitis B is provided by vaccination. In addition to the hepatitis B virus vaccine, a combination vaccine is also available that provides protection against hepatitis A.
The actual vaccination takes place according to different vaccination schedules. Usually it is necessary to undergo 3 injections at different time intervals. Ask your GP to prescribe and administer the vaccine.
Hepatitis C
Acute hepatitis C is a short-term infection. Symptoms can last up to 6 months. Sometimes your body can fight off the infection and the virus goes away.
Chronic hepatitis C is a long-lasting infection. Chronic hepatitis C occurs when the body is unable to fight the virus. About 75 to 85 percent of people with acute hepatitis C will develop chronic hepatitis C.
Early diagnosis and treatment of chronic hepatitis C can prevent liver damage. Without treatment, chronic hepatitis C can cause chronic liver disease, cirrhosis, liver failure, or liver cancer.
Groups of people at risk for hepatitis C:
- Injecting drug users.
- Blood transfusion or organ transplant before 1992.
- Patients with haemophilia and administered clotting factors before 1987.
- Dialysis patients.
- Working with blood or infected needles.
- Tattoos or piercings.
- Working or living in prison.
- Born to a mother with hepatitis C.
- HIV-infected.
- People with more than one sexual partner in the last 6 months or a history of a sexually transmitted disease.
- Men who have or have had sex with men.
- Sex partners of infected individuals.
Diagnosis of hepatitis C includes medical history, physical examination and blood tests to detect hepatitis C antibodies, hepatitis C RNA test, detection of the genotype of the virus.
Ultrasound examination is performed, and in rare cases a liver biopsy is necessary.
In the treatment of hepatitis C, the following drugs are used: pegylated interferon, antivirals - ribavirin, daclatasvir, elbasvir, ledipasvir, ombitasvir, dasabuvir. Treatment lasts 8-24 weeks and depends on the virus genotype, severity of liver damage, past treatment of hepatitis C.
How can I protect myself against viral hepatitis C?
There is no vaccination against hepatitis C, but it is still under development. Therefore, adherence to certain principles is necessary:
- Do not share drug needles or other drug materials.
- Wearing gloves if you have to touch another person's blood or open sores.
- The assurance that your tattoo artist or piercer uses sterile instruments and unopened ink.
- Do not share personal items such as toothbrushes, razors or nail clippers.
- Avoid promiscuous behaviour.
Hepatitis D
Hepatitis D virus is uncommon because infection can only occur when you have hepatitis B virus infection. In this way, hepatitis D is a double infection.
You can protect yourself from hepatitis D by getting the hepatitis B vaccine.
Acute hepatitis D is a short-term infection. The symptoms of acute hepatitis D are the same as those of any type of hepatitis and are often more severe.
Chronic hepatitis D is a long-lasting infection. Chronic hepatitis D occurs when your body is unable to fight off the virus and the virus does not go away.
People with chronic hepatitis B and D develop complications more often and more quickly than people who only have chronic hepatitis B.
Neonatal jaundice
Jaundice is the most common condition that requires medical care and hospitalization in newborns.
It affects up to 60-85% of mature newborns.
Yellow discoloration of the skin and sclerae in neonates with jaundice is the result of accumulation of unconjugated bilirubin. In most infants, unconjugated hyperbilirubinemia reflects a normal transient phenomenon.
However, in some infants, serum bilirubin levels may become excessively elevated, which may be a cause for concern because unconjugated bilirubin is neurotoxic and can cause death in newborns and lifelong neurological sequelae in infants who survive (kernicterus).
Risk factors for neonatal jaundice include:
- race: The prevalence is higher in East Asians and American Indians and is lower in Africans/African Americans.
- geography: The incidence is higher in populations living at high altitudes. Greeks living in Greece seem to have a higher prevalence than those living outside Greece.
- genetic and familial risk: The incidence is higher in infants with siblings who have had significant neonatal jaundice, and especially in infants whose older siblings have been treated for neonatal jaundice. The incidence is also higher in infants with mutations/polymorphisms in genes encoding enzymes and proteins involved in bilirubin metabolism and in infants with homozygous or heterozygous glucose-6-phosphatase dehydrogenase (G-6-PD) deficiency and other inherited haemolytic anaemias . Combinations of such genetic variants appear to exacerbate neonatal jaundice.
- nutrition: The incidence is higher in infants who are breastfed or receive inadequate nutrition. The mechanism of this phenomenon is not fully elucidated. However, if inadequate feeding volume is included, increased enterohepatic bilirubin circulation probably contributes to prolonged jaundice.
- maternal factors: Infants of mothers with diabetes have a higher incidence. Taking some medications may increase the incidence, while others decrease the incidence. Some herbal medicines taken by a breastfeeding mother can apparently worsen jaundice in an infant.
- birth weight and gestational age: The incidence is higher in preterm and low birth weight babies.
- congenital infection
Bilirubin values above 1.5 mg/dl (26 µmol/l) are considered abnormal. Jaundice becomes clinically evident at values above 5 mg/dl (86 µmol/l).
Treatment
The goal of treatment for unconjugated hyperbilirubinemia is to maintain bilirubin (Bi) concentrations in a range in which the risk of bilirubin neurotoxicity is low.
Causal treatment of hyperbilirubinemia is based on the management of the causative disease and is possible only after obtaining a correct diagnosis of the underlying disease after a thorough differential diagnostic analysis of the patient on the basis of history, clinical symptoms, laboratory and imaging investigations.
Symptomatic treatment includes optimization of enteral nutrition, phototherapy, exchange transfusion and pharmacological intervention.
Phototherapy reduces the concentration of bilirubin. It works on the principle of light degradation of bilirubin in the skin into non-toxic products, which are excreted from the body independently of liver function.
Light radiation of a certain wavelength acts on unconjugated bilirubin by converting it into a water-soluble form that can be excreted from the body in the urine.
Gilbert's syndrome
Gilbert's syndrome is not a disease in the classical sense; rather, it is a common and benign inherited variant of bilirubin metabolism that may be present in up to 6% of the population. The mutated gene is designated UGT1A1.
People with Gilbert's syndrome do not produce enough liver enzymes to keep bilirubin at normal levels. As a result, excess bilirubin builds up in the body - hyperbilirubinemia.
Symptoms
About 1 in 3 people with Gilbert syndrome have no symptoms. They learn they have the disease after blood tests are done for other conditions.
Among symptomatic patients, the most common feature is jaundice caused by elevated bilirubin levels in the blood. Jaundice can turn your skin and the whites of your eyes yellow, but it is not harmful.
Ľudia with Gilbert's syndrome also occasionally experience:
- Dark-colored urine or clay-colored stool.
- Difficulty concentrating.
- Dizziness.
- Gastrointestinal problems such as abdominal pain, diarrhea, and nausea.
- Fatigue.
- Flu-like symptoms, including fever and chills.
- Loss of appetite.
Diagnosis of the disease is focused on the typical clinical picture and blood tests:
- Liver function tests and measurement of bilirubin levels.
- Genetické testy na génovu mutáciu, ktorá spôsobuje Gilbertov syndróm.
Prognosis
Jaundice can cause a yellowish appearance that can be uniquely disturbing. However, jaundice and Gilbert's syndrome do not require treatment.
Gallstones
The gallbladder is a small pear-shaped organ on the right side of the abdomen, just below the liver. Its function is to store bile that is formed in the liver.
Stones forming in the gallbladder (cholecystolithiasis) can lead to pain in the right upper abdomen or in the middle in the stomach area.
You may experience gallbladder pain from time to time after eating high-fat foods such as fried foods, but the pain can occur at almost any time.
The pain caused by gallstones usually lasts only a few hours but can be severe.
If gallstones are left untreated or unidentified, symptoms may worsen and may include:
- high temperature
- rapid heartbeat
- yellowing of the skin and whites of the eyes (jaundice)
- itchy skin
- diarrhea
- chills
- confusion
- loss of appetite
The above symptoms arise when the gallbladder is inflamed, when gallstones travel into the bile ducts (choledocholithiasis) or when pancreatitis (inflammation of the pancreas) develops.
Gallbladder stones can be cholesterol stones, which are formed when there is an excess of cholesterol, or pigment stones, which are formed when there is an excess of bilirubin. Small stones with thickened bile in the gallbladder are called gallbladder sludge or sludge.
Diagnosis is based on abdominal ultrasound or abdominal CT scan, radionuclide scan of the gallbladder in unclear cases, and laboratory examination with findings of hyperbilirubinemia (elevated bilirubin level) and elevated liver parameters.
Treatment
In the medical treatment of asymptomatic patients, bile-thinning drugs (deoxycholic and ursodeoxycholic acids) are used, in pain spasmolytics (cramp-relieving drugs) and analgesics (painkillers) are used, in inflammation antibiotic treatment is used.
A stuck stone in the bile duct should be addressed by ERCP (endoscopic retrograde cholangioscopy), which both identifies the stone and can remove it.
Ultrasonic stone breaking (lithotripsy for little success is on the decline. When there are many stones in the gallbladder, the most commonly performed removal of the gallbladder is cholecystectomy, which is done laparoscopically.
How it is treated: Jaundice
Treatment of jaundice
Show moreJaundice is treated by
Other names
Interesting resources










